 Has a means of communication been established in case of a problem (e.g., exposure, spill, breakage, fire, etc.)?.Consider the specifics of the area you will be inspecting and wear the personal protection equipment (PPE) required in that area. Ideally, the inventory should be conducted by a team of two persons (one can write and the other can handle the products if needed). Set a path to follow so that there are no missed products or locations. When doing an inventory, it is useful to have a floor plan where to mark the areas where chemicals or products are used or stored. What are general steps to follow when conducting a chemical or product inventory? Back to top Evaluate if the training provided to workers matches the products on site.During preparation, other items related to chemical safety can be inventoried, including safety data sheets (SDS), personal protective equipment (PPE), and emergency spill response supplies.Collect usage and waste data for the annual National Pollutant Release Inventory (NPRI) and other jurisdictional toxic substance or emissions reports.Meet integrated management system requirements (e.g., ISO, COR, or other auditing requirements).Comply with occupational health and safety (OHS) and environmental regulations.Identify locations needed for emergency response procedures and the municipal fire plan.Identify products that could be replaced with safer alternatives.Remove products that are expired or no longer used.Verify that hazardous products are being stored correctly and safely.Performing a periodic inventory can have several benefits: Why should a chemical or product inventory be done? Back to top Although not a formal recommendation, the OIG also called on VHA to report any data limitations until corrections can be made.You are here: Inspection Checklist - Sample Checklist for Chemical or Product Inventory VHA concurred with the OIG’s two recommendations to provide guidance for reporting expired quantities of PPE that may still be of use, and to more effectively verify facilities’ self-reported information. The OIG found, however, that VHA could improve the accuracy and consistency of the PPE data for reporting and monitoring. Overall, the OIG found VHA took swift steps to work around known limitations in its inventory management system by developing new processes and tools, to use near real-time information on PPE inventory to shift and order supplies, and to otherwise ensure its facilities would not run out of PPE. Some individuals reported running low, but risks of outages were mitigated by shifting supplies among facilities or acquiring additional PPE in time. In interviews of 22 people involved in logistics operations at 42 facilities, no one reported running out of PPE items. Without reliable PPE inventory information, VHA cannot effectively assess demand, monitor stock levels, or identify supply shortages that require prompt action. The review team also solicited information about whether facilities ran out of PPE or experienced significant shortages. 
The OIG assessed how VHA reported and monitored PPE supply levels during the pandemic.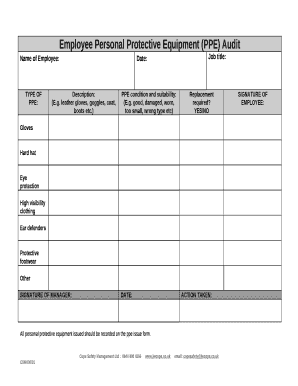 
The VA Office of Inspector General (OIG) received hotline allegations that VHA medical facilities could not acquire and maintain enough PPE to keep pace with escalating needs. As the nation’s largest integrated healthcare system, the Veterans Health Administration (VHA) had to compete for PPE for its personnel and patients. The spread of COVID-19 drastically increased the demand for personal protective equipment (PPE) such as masks, gloves, and gowns, and significantly disrupted the global supply chain. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
